Patient safety is main concern
Other considerations:
- Periods of transition can be associated with a deterioration in clinical performance
- Serious performance issues are rare
- NB these often have a complex background
- Take advice and seek support
General Principles
- Early identification of problems and intervention is essential
- Disappearing
- low work act
- ward rage
- Rigidity
- bipass syndrome – nurses and juniors avoid seeking the doctors opinion
- Career problems
- Insight failure
- lack of engagement in educational processes
- Lack of initiative/appropriate professional engagement
- inappropriate attituesa
- Establish and clarify the circumstances and facts as quickly as possible
- Remember poor performance is a ‘symptom not a diagnosis’
- explore the
- clinical performance of the individual
- personality and behavioural issues
- sickness/ill health
- environmental issues
- If correct diagnosis made, can get effective remediation
- Document clearly
- Communicate misgivings
- explore the
Traffic light framework
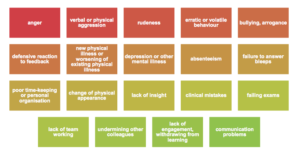
A Diagnostic framework…

Advice to manage
- Clinical performance
- focused retraining
- extended period of clinical supervision
- Personality and behavioural issues
- clinical supervision
- developmental mentoring
- Feedback using video etc
- Health issues
- Environmental issues
- lack of resources
- unrealistic work demands
- poor clinical management
- poor support
- substandard working environments
HEKSS Trainee Support Guide
Concerns may come through a number of ways…
- professional examinations
- regular NHS appraisals
- assessments
- clinical governance frameworks
- clinical audit activities
- litigation
- information from colleagues
- Explore concerns
Unless serious, educational supervisor is best placed to deal with initial concerns
Also need to discuss with TPD
Should also discuss with the trainee in order to get their perspective
- Agree a plan (SMART)
Record the meeting and plan advised
SMART:
Specific
Measurable
Achievable
Realistic
Time scale
3. Pass on information
To the deanery
- Address issues

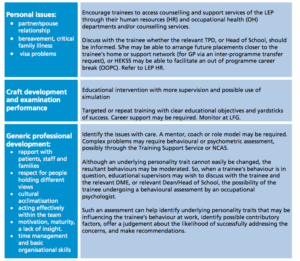


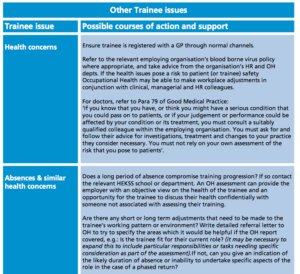


Good record keeping
Trainee should be made aware of any discussions and should be given a copy of any documentation
Trainees in difficulty should be discussed at LFG
Role of Supervisor
- Address the issue as soon as possible
- take more formal steps if any concern about patient safety
- look beyond to try to establish the underlying cause
- focus on evidence and facts
- share information on a need to know basis
Employer
needs to deal with employment issues inc performance, grievance, discrimination, whistleblowing and potential disciplinary matters are dealt with appropriately
HEKSS should be informed if
- progression is likely to be affected
- issues which may have an impact on revalidation
- additional funding required
- trainees at risk of receiving an unsatisfactory outcome at ARCP
TSS offers guidance and retraining
3 tiers of support
- Educational supervisors in each of trusts +/- College Tutors
- Programme leads/DMEs
- HEKSS careers team
Doctor in difficulty: locum (my own strategy)
- Checks before:
- Ideally use Dr known to department – either trust bank or previous trainee
- CV
- Using a reputable agency
- Ensure no current issues/concerns before employing
- Some departments have policy to employ locum initially during the day to ensure that is supervised before allowing to work the night
- If problem has occurred
- Pull notes of the patient plus others which (s)he has seen
- Is there a clinical issue
- Pure clinical
- Poor communication
- Missunderstanding
- Blind spot/lack of knowledge
- Not listening to advice given (I would classify this as the most serious)
- Probity
- Consider if should continue to work in the department until this has been resolved
- If suspending them, inform other consultants!
- Work with supervision?
- Day shifts only?
- Inform the RO for the agency to ensure that they are aware and can address this training need
Consultant colleague in difficulty
Less likely to come up in viva as usually dealt with by clinical lead
However key features include
- Patient safety is paramount
- Discretion
- Responsible officer
- Occupational Health where appropriate
When should a Dr be suspended?
Haven’t managed to find a reference for this
- If involved in a SI/never event?
- Lots of incidents
- Locum
- Any other ideas?